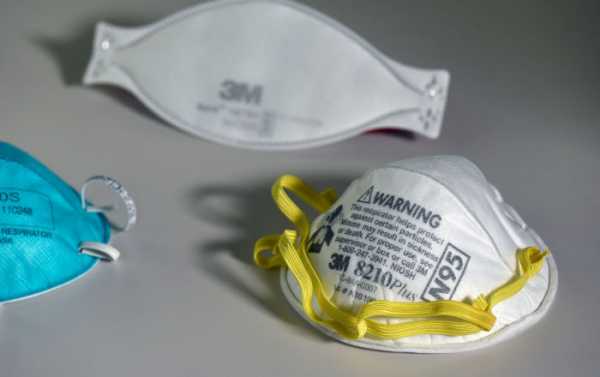
A new study published in the journal JAMA finds that reusable elastomeric half-mask respirators (EHMRs) worn frequently by those in the construction and manufacturing industries are a suitable alternative to N95 masks, which are used to protect health care workers from pathogens and are currently in short supply due to the COVID-19 pandemic.
The study was conducted by researchers at the National Institute for Occupational Safety and Health at the US Centers for Disease Control and Prevention (CDC), Emory University, the Baylor College of Medicine and the University of Texas Health Science Center. The findings, published on March 25, revealed that the time it takes to fit and train healthcare personnel to use disposable N95 respirators is about the same time it takes to train them for reusable EHMRs.
“Training and fit testing health care providers on respirators can be time consuming, and in an epidemic we want to train and fit test a large number of workers quickly,” first author Lisa Pompeii, professor of pediatrics – epidemiology at Baylor, said in a March 27 news release.
“Our study shows that training and fit testing workers on these reusable respirators does not represent a barrier for possible use by hospitals. An advantage of reusable respirators is that there is no need to stockpile them,” Pompeii added.
However, the study also concluded that a deeper understanding of how to best disinfect EHMRs is necessary before they are widely used in healthcare settings.
“Major distributors in the United States have reported shortages of PPE, specifically N95 respirators, facemasks, and gowns. Health care facilities are responsible for protecting their HCP [healthcare providers] from exposure to pathogens, including by providing appropriate PPE,” the CDC explains on its website.
“In times of shortages, alternatives to N95s should be considered, including other classes of FFRs [filtering facepiece respirators], elastomeric half-mask and full facepiece air purifying respirators, and powered air purifying respirators (PAPRs) where feasible. Special care should be taken to ensure that respirators are reserved for situations where respiratory protection is most important, such as performance of aerosol-generating procedures on suspected or confirmed COVID-19 patients or provision of care to patients with other infections for which respiratory protection is strongly indicated (e.g., tuberculosis, measles, varicella),” the CDC adds.
“We are the richest country in the world, and yet we can’t protect our health care providers when fighting the deadliest virus we’ve dealt with in most of our lifetimes,” Ryan Stanton, an American College of Emergency Physicians board member who works at a hospital in Lexington, Kentucky, told Bloomberg. “There’s a significant level of distrust with physicians and nurses and others because we feel the requirements and suggestions for PPE are being downgraded because of availability and not because of science.”
Usually, PPE like N95 masks and gowns are discarded after one use. However, many health care workers are having to reuse equipment for days on end due to the shortages. According to 56-year-old Karine Raymond, a nurse at the Montefiore Health Center in New York City’s Bronx borough, conditions are so dire that she is considering writing her will.
“We’re doing the best we can. We’re trying hard to try and help these poor souls without unduly opening ourselves up to anything dangerous. If we go down, then there’s nobody left to care for the patients, is there?” she said.
Sourse: sputniknews.com